
A new look at an old protein may yield therapy for contagious respiratory disease
Researchers at UC Santa Barbara have identified the mechanism by which pathogenic Bordetella bacteria promote the colonization of mammalian airways. This mechanism, if interrupted, could lead to novel therapies for diseases such as whooping cough (pertussis) in humans and kennel cough in dogs.
“For a long time, it wasn't exactly clear how the bacteria bind to the cells in our respiratory tracts,” said Michael Costello, a postdoctoral researcher in the lab of UCSB microbiologist Christopher Hayes. This binding is the first step by which Bordetella colonize our airways; understanding this mechanism may lead to insights into strategies to defeat these bacteria.
The research, largely supported by the National Institutes of Health, is published in the journal Science.
A ‘molecular grappling hook’
Whooping cough and its canine cousin, kennel cough, are highly contagious respiratory diseases brought on by the airborne Bordetella bacteria. Both are characterized by distinctive and severe “whooping” or “honking” coughs. Both can affect all ages of their hosts, but the very young, very old or immunocompromised are the most vulnerable. Vaccines for the diseases have been around for about a century, though their effectiveness declines rapidly over the course of a few years.
“People have been working on this organism since the 1920s,” Costello said, “and early on they realized that there is one protein critical for colonizing a host’s respiratory tract, but no one really understood the mechanics of how it mediates adhesion to our cells.”
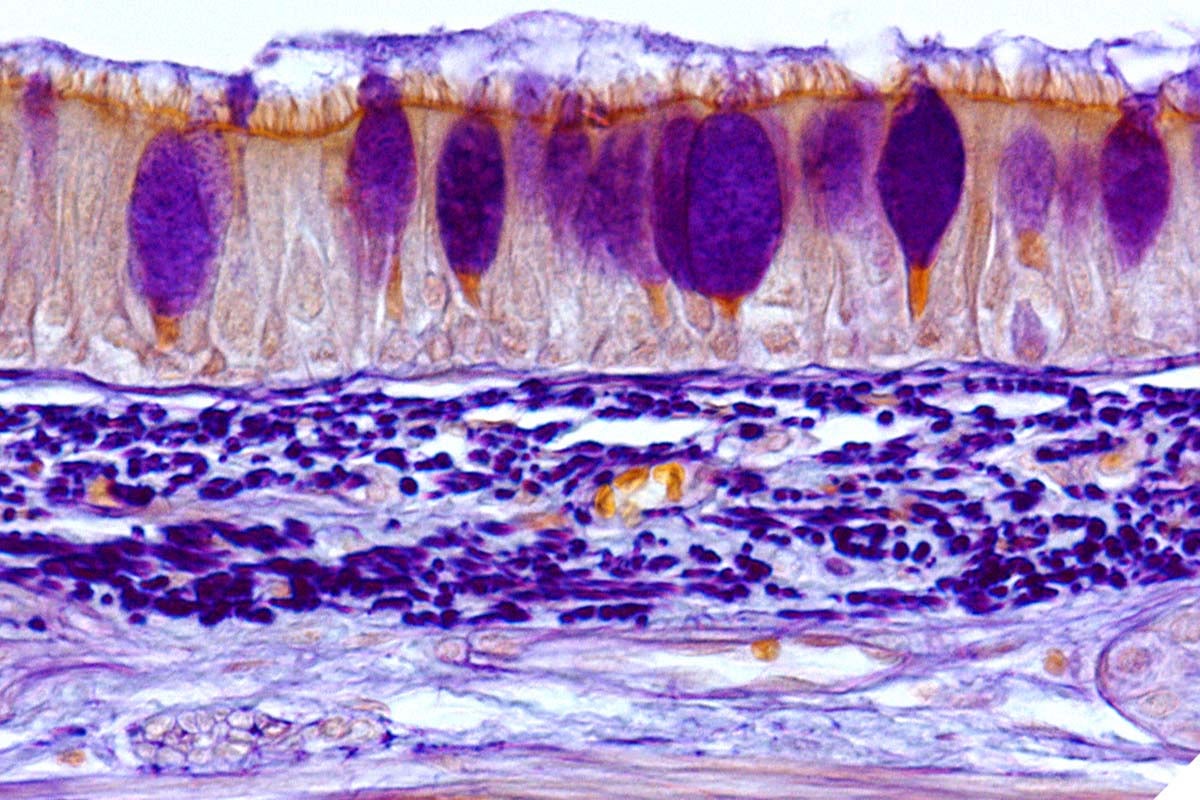
This lack of clarity stems largely from the fact that the mammalian respiratory system is highly evolved to clear the airways by trapping and sweeping away foreign objects, thanks to a layer of mucus that traps foreign bodies — from dust particles to pathogens — atop a constantly beating layer of hairlike projections called cilia. The question was, how do these bacteria manage to bypass that defense?
The team had a suspect: a protein secreted by the bacteria called the filamentous hemagglutinin (FhaB) adhesin. They discovered that FhaB carries a small region that binds to the microtubule network found inside motile cilia. Although FhaB has long been known to be important for Bordetella infection, previous research largely focused on how FhaB is converted into a smaller "mature" fragment.
“This is a very large protein,” Hayes said. “And when people looked for it in the pathogen, they found it was broken down into a smaller protein. This smaller fragment lacks the region that binds to microtubules." Since the 1990s researchers have thought that this fragment was the mature form of the adhesin, he said, “not realizing that they were overlooking an essential part of the bacteria’s strategy.”
However, Hayes and fellow microbiologist David Low (also an author on this paper) had been studying distantly related proteins that are involved in bacterial competition.
“These antibacterial proteins intoxicate other cells by moving a toxic cargo into their neighbor,” Costello said. “And so we explored this framework, this idea that the adhesin could be translocating a toxic cargo.”
With advanced techniques, including cryo-electron microscopy, fluorescence microscopy and genetic modification, the researchers examined this protein and found that its cargo wasn’t toxic. Instead, they discovered that FhaB delivers a domain that binds tightly to the internal microtubule cytoskeleton of cilia.
“We think it works as a molecular grappling hook,” Costello said. With the bacteria anchoring themselves to the cilia so they can resist the flow of the mucus.
But that’s not all. “It looks like this protein allows them to walk down the cilia to the base, where they are less likely to be removed from the airway,” Hayes said.
As damaging as these bacteria may be, the researchers suspect that the pathogens aren’t trying to invade the airway cells they stick to.
“From my understanding, they’re not an intracellular pathogen so they don’t necessarily want to invade the host cells,” said Mia Raimondi, a senior undergraduate research assistant in the Hayes lab. “They just want to hang out there and have a safe space to divide and grow before finding another human or dog.”
This knowledge opens the door to potential therapeutic strategies for defeating the bacteria, and also raises further questions: Exactly how do bacteria manage to penetrate to the base of the cilia? How do they make it back out past the layer of mucus? How do they know when to deploy their molecular grappling hooks? Are other proteins required for the initial adhesion to cilia?
“We know there's another adhesin that’s also important for this process,” Raimondi added. She’s studying how hairlike projections from the bacterium, called fimbriae, might work in this newly discovered process, and how these proteins recognize cilia.
“This is clearly a complex process, and there’s much still to learn,” commented Hayes.
Research on this project was also conducted by Fernando Garza-Sánchez, Jacob A. Torres, Nickolas Holznecht, Jessica Mendoza, Thomas Weimbs, Meghan Morrisey and Diego Acosta-Alvear at UCSB; Bryan Neumann, Bonnie J. Cuthbert, Sasiprapa Prombhul, Celia W. Goulding and Shane Gonen at UC Irvine; and Jana Holubova, Abdul Samad, Ladislav Bumba, Ondrej Stanek and Peter Šebo at the Czech Academy of Sciences.




