A New Old Therapy

The fight against drug-resistant pathogens remains an intense one. While the Centers for Disease Control’s (CDC) 2019 “biggest threats” report reveals an overall decrease in drug-resistant microbe-related deaths as compared to its previous report (2013) the agency also cautions that new forms of drug-resistant pathogens are still emerging.
Meanwhile, the options for treating infections by these germs are diminishing, confirming doctors’ and scientists’ worries about the end of the age of antibiotics.
“We knew it was going to be a problem early on,” said UC Santa Barbara chemistry and biochemistry professor Irene Chen. “Basically as soon as penicillin was discovered, a few years later it was reported that there was a resistant organism.” Thanks to factors such as horizontal gene transfer and rapid reproduction, organisms such as Gram-negative bacteria are able to evolve faster than we can produce antibiotics to control them.
So Chen and her research group are seeking alternatives to antibiotics, in a growing effort to head off the tide of incurable bacterial infections. In their work, the group has turned to bacteriophages, a naturally occurring group of viruses that colonize on bacteria.
“That’s their natural function, really, to grow on and kill bacteria,” said Chen, author of a paper that appears in the Proceedings of the National Academy of Sciences. By taking advantage of the bacteriophages’ ability to home in on specific bacteria without damaging the rest of the microbiome, the researchers were able to use a combination of gold nanorods and near-infrared light to destroy even multidrug-resistant bacteria without antibiotics.
Phage therapy isn’t new, Chen said. In fact, it has been used in the former Soviet Union and Europe for about a century, though they are seen largely as last-resort alternatives to antibiotics. Among the unresolved issues of phage therapy is the incomplete characterization of the phages’ biology — a biology that could allow for unintended consequences due to the phages’ own rapid evolution and reproduction, as well as potential toxins the viruses may carry. Another issue is the all-or-nothing aspect of phage therapy, Chen added.
“It’s difficult to analyze the effect of a phage treatment,” she said. “You might see it completely work or you might see it completely fail, but you don’t have the kind of dose response you want.”
To surmount these challenges, the Chen lab developed a method of controlled phage therapy.
“What we did was to conjugate the phages to gold nanorods,” she explained. These “phanorods” were applied to bacteria on in-vitro cultures of mammalian cells and then exposed to near-infrared light.
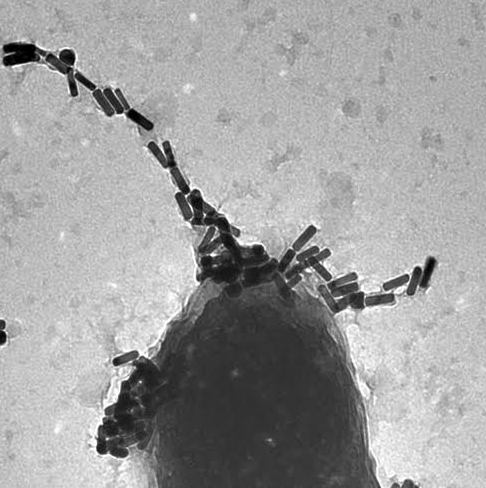
Conjugated to phages,gold nanorods find their target: a bacterial cell wall
Photo Credit: COURTESY IMAGE
“When these nanorods are photo-excited, they translate the energy from light to heat,” Chen said, “and that creates very high local temperatures.”
The heat is enough to kill the bacteria, and it also kills the phages, preventing any unwanted further evolutions. The result is a guided missile of targeted phage therapy that also allows for dosage control. The lab found success in destroying E. coli, P. aeruginosa and V. cholerae — human pathogens that cause acute symptoms if left unchecked. They also were able to successfully destroy X. campestris, a bacteria that causes rot in plants.
In a collaboration with UC Santa Barbara mechanical engineer Beth Pruitt, the lab determined that while the heat successfully destroyed bacteria and phage, more than 80% of the mammalian cell culture underneath the bacteria biofilm survived.
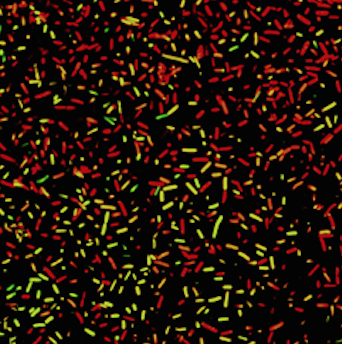
Bacteria under fire: Green bacteria are alive, while the red ones are dead
Photo Credit: COURTESY IMAGE
“This issue of whether it damages mammalian tissues is very important,” Chen said. “Work in nanotechnology and nanomedicine treating bacterial infections indicates that when it’s non-targeted, it really does burden the surrounding tissues.”
The lab plans to investigate other possible phages to counter other bacteria, possibly engineering a photothermal method that could treat multiple bacterial infections.
Research on this study was conducted also by UCSB postdoctoral fellow Huan Peng (lead author), Raymond E. Borg and Liam P. Dow.



